 Gastric Bypass Mobile, AL
Gastric Bypass Mobile, AL
SAMPA surgeons performed the first laparoscopic Roux-en-Y gastric bypass in the region in March 2001
The gastric bypass, also referred to as the Roux-en-Y, or RNY, for how it is performed, was first introduced several decades ago. Until recently, the bypass was the most popular weight loss surgical procedure in the United States because of its exceptional weight loss and disease resolution potential. The gastric bypass employs a combination of restriction and malabsorption performed in a laparoscopic or minimally invasive manner.
How The Gastric Bypass Is Performed
Since the gastric bypass is performed in a minimally invasive manner, the large single incisions of old are no longer needed. Instead, much like other bariatric procedures we offer, five small abdominal incisions are used. Proven benefits of minimally invasive surgery include a shorter hospital stay, less pain and blood loss, and generally, fewer complications.
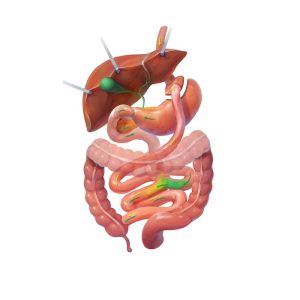
During surgery, the surgeon cuts approximately 80% of the existing stomach. The remaining, small gastric pouch is about as big as a golf ball and holds very little food. This is the restrictive portion of the procedure. Unlike the gastric sleeve, a gastric bypass leaves the larger portion of the stomach within the abdomen, which continues to produce gastric juices.
The second part of the surgery involves bypassing part of the small intestine. This reduces the number of calories that can be absorbed through the sensitive intestinal lining and represents the malabsorptive portion of the gastric bypass. The lower portion of the bypassed intestine is connected directly to the small stomach pouch. The upper portion of the bypassed intestine remains connected to the larger stomach pouch while the other end is re-connected lower down in the small intestine to allow gastric juices to mix.
Recovery and Results of the Gastric Bypass
The gastric bypass requires a hospital stay of two to three nights for most patients, assuming an uneventful surgery and post-op recovery.
Gastric bypass results are generally excellent, with exceptional short-to mid-term excess bodyweight loss potential of up to 80%. Over the long-term, results are similar to the gastric sleeve and patients typically maintain >50% of their excess body weight, also improving or resolving most of the diseases associated with obesity. Results will vary between patients.
Meet Dana, A Gastric Bypass Patient
Benefits of the Gastric Bypass
- Decades of proven weight loss and clinical research
- Less pain, blood loss, and shorter hospital stay as a result of the procedure being performed laparoscopically or robotically
- Exceptional weight loss and disease resolution or improvement potential
- Particular improvement in patients with type-2 diabetes, GERD, and sleep apnea
- No permanently implanted medical device as compared to gastric band
Risks and Considerations of the Gastric Bypass
- Post-surgical diet is more restrictive than other bariatric procedures
- Patients may experience an uncomfortable but not life-threatening condition known as dumping syndrome if they consume high-fat or sugary foods in excess
- Patients will have to take a multi-vitamin for the rest of their lives and may experience nutritional deficiencies requiring supplementation including Vitamin B12, Calcium, Vitamin D, and/or Iron to name a few
- In rare cases, the staple line used to seal the separated stomach may leak
- The risks associated with a major surgical procedure include infection, pain, blood loss, and in rare cases death
- Weight regain can occur if the post-op diet or exercise program is not followed and the gastric pouch begins to dilate.
The gastric bypass is not appropriate for all patients, however it has been considered the gold standard in bariatric surgery for decades. Watching our online seminar, followed by a consultation with one of our surgeons is the best way to understand if the gastric bypass is ideal for your particular circumstance.


 Other Weight Loss Surgeries / Procedures
Other Weight Loss Surgeries / Procedures